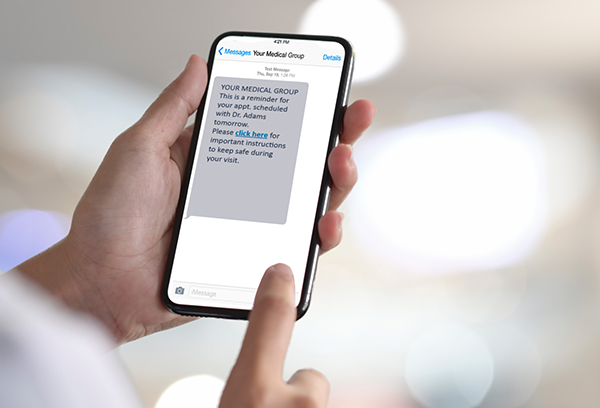
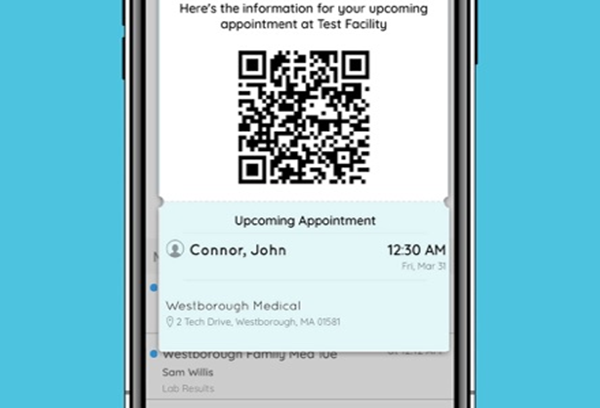
COVID-19: Outpatient Toolkit
As you prepare to resume outpatient services, there are several considerations and opportunities to improve the safety of your staff and patients. Array has developed a consolidated toolkit to reduce infection risk, acknowledge and ameliorate patient and staff anxiety, and streamline patient throughput. We have also included links to expanded resources and sample products to support your teams.